Do you sedation for transcutaneous pacing?
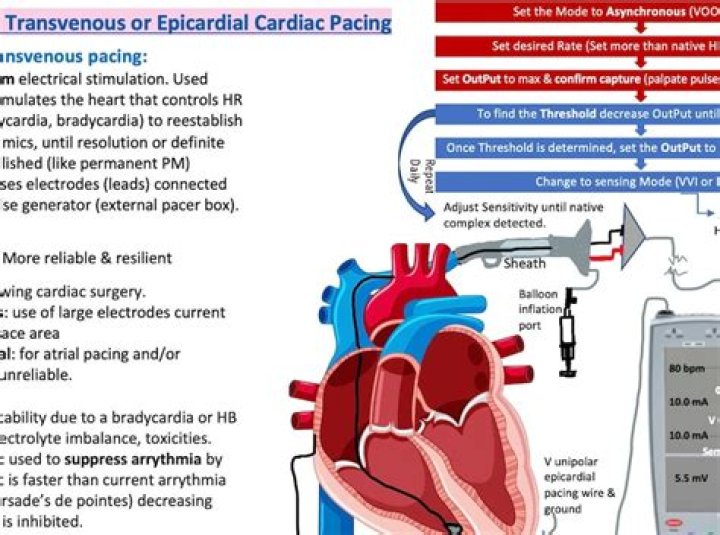
Transcutaneous cardiac pacing may be associated with discomfort such as a burning sensation of the skin, skeletal muscle contractions, or both. Because of this, patients who are conscious and hemodynamically stable should be sedated with a drug, such as midazolam, before initiation of pacing (see Procedural Sedation).
How is transcutaneous pacing done?
Transcutaneous Pacing (TCP) is a temporary means of pacing a patient’s heart during an emergency and stabilizing the patient until a more permanent means of pacing is achieved. It is accomplished by delivering pulses of electric current through the patient’s chest, stimulating the heart to contract.
Why atropine does not work on heart blocks?
Since atropine’s effect is primarily on the SA node in the atria, a 3rd-degree block would prevent its effect on the SA node from influencing the rate of ventricular contraction which is needed to improve perfusion.
Is dopamine used for bradycardia?
Dopamine can be very effective in treating hypotension with signs and symptoms of shock. Dopamine is typically used as a second line drug for symptomatic bradycardia after atropine.
How fast do you push IV atropine?
Administer Atropine 0.5 mg IV repeating every 3-5 minutes to a total dose of 3 mg IV, until a heart rate of greater than 60/minute is reached. 3. Transcutaneous pacing (TCP) when available may be initiated prior to establishment of IV access and/or before Atropine begins to take effect.
How do you give atropine?
Atropine is administered by intravenous injection or intramuscular injection. Other pharmaceutical forms/strengths may be more appropriate in the cases where a dose above 0.5 mg is required. All these contra-indications are however not relevant in life-threatening emergencies (such as bradyarrhythmia, poisoning).
What rhythms can you pace?
For pacing readiness (i.e. standby mode) in the setting of acute myocardial infarction (AMI) with the following:
- Symptomatic sinus bradycardia.
- Mobitz type II second-degree AV block.
- Third-degree AV block.
- New left, right or alternating bundle branch block or bifascicular block.
What is the difference between transcutaneous pacing and transvenous pacing?
It can be used to treat symptomatic bradycardias that do not respond to transcutaneous pacing or to drug therapy. Transvenous pacing is achieved by threading a pacing electrode through a vein into the right atrium, right ventricle, or both….
| Transvenous pacing | |
|---|---|
| Specialty | cardiology |
Does atropine increase BP?
However, when given by itself, atropine does not exert a striking or uniform effect on blood vessels or blood pressure. Systemic doses slightly raise systolic and lower diastolic pressures and can produce significant postural hypotension.
Can paramedics give atropine?
Yes, the atropine auto-injector comes in both an adult dose and a pediatric dose.
What is the appropriate pacing rate for TCP?
TCP should be started at a rate of 60/min. Adjust up or down depending on the patient’s response. Assess response using the femoral pulse rather than the carotid pulse as muscle movements resulting from TCP may affect the latter. Consider using dopamine (2 to 20 µg/kg each min) or epinephrine (2 to 10 µg per min) where the pacing is not sufficient.
How much dopamine do you give for transcutaneous pacing?
Consider using dopamine (2 to 20 µg/kg each min) or epinephrine (2 to 10 µg per min) where the pacing is not sufficient. These actions should be enacted in rapid succession, and in cases even simultaneously, to prevent cardiac arrest. What is transcutaneous pacing (TCP)?
What are the pacing guidelines for atropine administration?
If signs of severely poor perfusion are present, do not delay pacing to administer atropine. TCP should be started at a rate of 60/min. Adjust up or down depending on the patient’s response. Assess response using the femoral pulse rather than the carotid pulse as muscle movements resulting from TCP may affect the latter.
How to prepare for transcutaneous pacing in patients with poor perfusion?
If the patient has poor perfusion, preparation for transcutaneous pacing should be initiated, and an assessment of contributing causes (H’s and T’s) should be carried out. Click below to view the bradycardia algorithm diagram. When finished, click again to close the diagram. Bradycardia Algorithm Diagram or Download the High Resolution PDF Here.