How can you tell the difference between APML and AML?
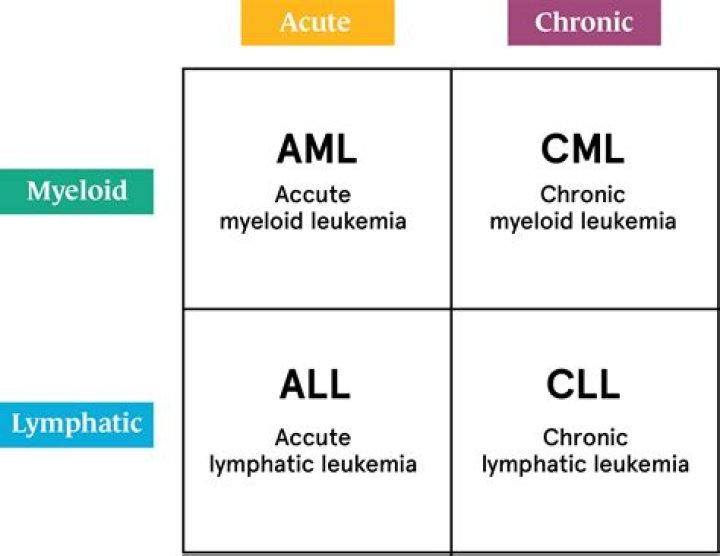
Acute promyelocytic leukaemia (APML) is a rare sub-type of acute myeloid leukaemia (AML) and is sometimes referred to as AML M31. APML accounts for only 10% of all AML diagnoses. In APML, immature abnormal neutrophils (a type of white blood cell) known as promyelocytes accumulate in the bone marrow.
How is APML diagnosed?
APML is diagnosed by examining samples of your blood and bone marrow.
- Full blood count. The first step in diagnosis is a simple blood test called a full blood count (FBC) or complete blood count (CBC).
- Bone marrow examination.
- Further testing.
- Other tests.
What are the peripheral blood smear findings in acute myeloid leukemia?
(A) Peripheral blood smear shows a large blast with Auer rods in the cytoplasm (Wright-Giemsa stain, ×1,000). (B) Bone marrow aspirate smear shows large blasts with irregular nuclear contours (Wright-Giemsa stain, ×1,000).
How does ATRA work in APML?
All-Trans Retinoic Acid (ATRA) ATRA targets and eliminates the PML/RARα abnormality. This treatment causes a marked decrease in the concentration of leukemic blast cells in the marrow, and a remission frequently follows. Used alone, ATRA can induce a short-term remission in at least 80 percent of patients.
Can Apml come back?
The prognosis of acute promyelocytic leukemia (APL) has been improved by the combination of all-trans retinoic acid (ATRA) with chemotherapy. Nonetheless, relapse occurs in a certain proportion of patients, mostly within three to four years after treatment.
Is promyelocytic leukemia curable?
Because of advances in diagnostic techniques and modern treatments, APL is today considered to be the most curable subtype of acute myeloid leukemia in adults, with complete remission rates of 90 percent and cure rates of approximately 80 percent and even higher among low-risk patients.
What does a peripheral blood smear show?
It evaluates the white blood cells (WBCs, leukocytes), red blood cells (RBCs, erythrocytes) and platelets (thrombocytes). Blood smear is examined to investigate hematological problems (disorders of the blood) and, occasionally, to look for parasites within the blood such as malaria and filaria.
Can Apml be cured?
Acute promyelocytic leukemia (APL) has become a curable disease by all-trans retinoic acid (ATRA)-based induction therapy followed by two or three courses of consolidation chemotherapy. Currently around 90% of newly diagnosed patients with APL achieve complete remission (CR) and over 70% of patients are curable.
How long do you live with AML?
Outlook for AML They come from the National Cancer Intelligence Network (NCIN). Generally with AML, around 20 out of 100 people (around 20%) will survive their leukaemia for 5 years or more after their diagnosis.
What does a bone marrow aspirate show in non-APL AML?
This bone marrow aspirate represents a patient with non-APL AML and shows a marked shift to immaturity that could be easily mistaken for APL. Almost all of the cells are promyelocytes with prominent cytoplasmic granulation.
How is acute promyelocytic leukemia (APL) characterized?
Acute promyelocytic leukemia is characterized by the presence of the large atypical promyelocytes and other myeloid precursors in various stages of development in the peripheral blood. The bone marrow is hypercellular, and APL promyelocytes account for about 30% of the myeloid cells in the classic variant.
What are the morphologic features of microgranular acute promyelocytic leukemia (M3V)?
This blood smear shows characteristic morphologic features of microgranular acute promyelocytic leukemia (M3V). A prominent leukocytosis is present with numerous cells exhibiting bilobed or monocytoid-appearing nuclei. Cytoplasmic granulation is absent to inconspicuous. Rare cells contained Auer rods (not shown in this field). Wright-Giemsa stain.
What are the clinical indications for peripheral blood film analysis?
Common clinical indications for peripheral blood film analysis include unexplained cytopenia: anaemia, leucopenia or thrombocytopenia; unexplained leukocytosis, lymphocytosis or monocytosis;