Is there a cure for pellucid marginal degeneration?
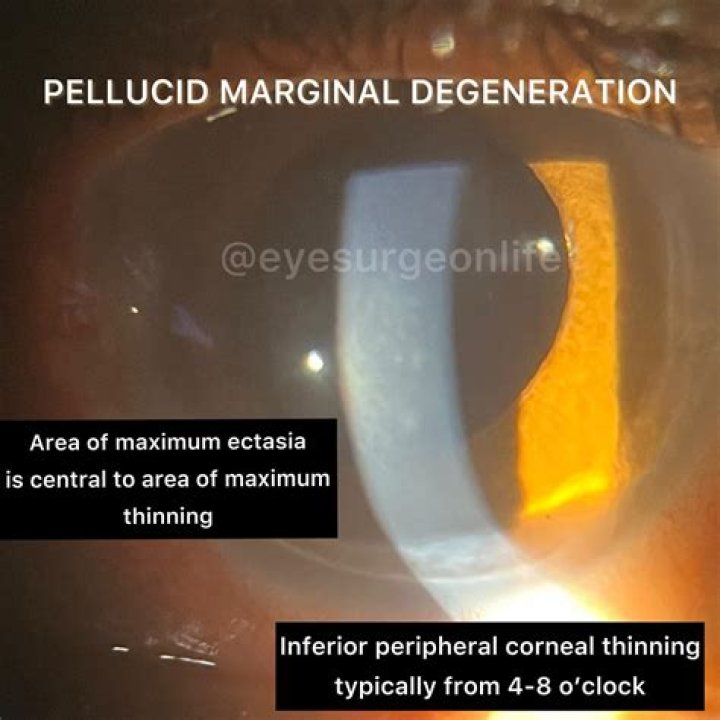
Pellucid marginal degeneration is diagnosed by corneal topography. Corneal pachymetry may be useful in confirming the diagnosis. Treatment usually consists of vision correction with eyeglasses or contact lenses. Intacs implants, corneal collagen cross-linking, and corneal transplant surgery are additional options.
Is pellucid marginal degeneration progressive?
Pellucid marginal degeneration (PMD) is a bilateral (may be asymmetric), progressive, inferior crescentic peripheral thinning of the cornea.
Is pellucid marginal degeneration rare?
Pellucid marginal corneal degeneration (PMD) is a rare ectatic disorder which typically affects the inferior peripheral cornea in a crescentic fashion. The condition is most commonly found in males and usually appears between the 2nd and 5th decades of life affecting all ethnicities.
Why is eye transplanted cornea grafted?
A deep anterior lamellar transplant (DALK) procedure is used when cornea damage extends deeper into the stroma. Healthy tissue from a donor is then attached (grafted) to replace the removed portion. Artificial cornea transplant (keratoprosthesis).
Is pellucid marginal degeneration bilateral?
Pellucid marginal degeneration (PMD) is a rare bilateral corneal disorder characterised by thinning in the peripheral portion of the inferior cornea with marked steepening just superior to the thinned zone.
How common is pellucid marginal degeneration?
Pellucid marginal degeneration appears to be a rare entity. Tummanapalli et al surveyed 1,113 patients who had corneal ectasias; they found that of these, only 3% had PMD while the remaining 97% had keratoconus.
What is corneal degeneration?
Corneal degenerations are changes or gradual deteriorations in the tissue of the cornea. They can negatively impact the function of the cornea, limiting its ability to help the eye focus properly. Over time, corneal degenerations can cause loss of vision, eye pain, and other issues.
Are cornea transplants successful?
A cornea transplant can restore vision, reduce pain, and improve the appearance of a damaged or diseased cornea. Most cornea transplant procedures are successful. But cornea transplant carries a small risk of complications, such as rejection of the donor cornea.
Is pellucid marginal degeneration caused by peripheral corneal thinning?
Abstract Pellucid marginal degeneration (PMD) is an uncommon cause of inferior peripheral corneal thinning disorder, characterized by irregular astigmatism. We analyzed a case of bilateral PMD patient and treated one eye with corneal collagen cross-linking (CXL) therapy.
What are the treatment options for progressive pellucid marginal degeneration (PRM)?
Pellucid marginal degeneration is diagnosed by corneal topography. Corneal pachymetry may be useful in confirming the diagnosis. Treatment usually consists of vision correction with eyeglasses or contact lenses. Intacs implants, corneal collagen cross-linking, and corneal transplant surgery are additional options.
How do you diagnose keratoconus and pellucid marginal degeneration?
Corneal Topography is the gold standard for diagnosing both Keratoconus and Pellucid Marginal Degeneration, as well as differentiating the two conditions. Keratoconus has a very characteristic “cone” shaped area of thinning and bulging as seen with corneal topography.
Why don’t hard lenses work for pellucid marginal degeneration?
Since the area of thinning is so peripheral with Pellucid Marginal Degeneration, small diameter hard lenses like the Rose 2K are not effective. Their small size causes these lenses to slide too far down over the “beer belly.” Instead, very large diameter hard lenses called Scleral Contact Lenses (seen above) are the standard of care.