What is the guideline for transfusion rates of platelets?
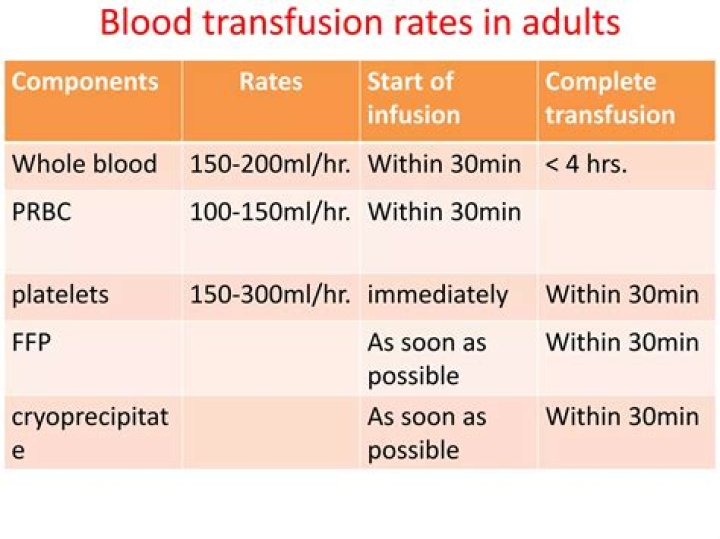
Consider increasing the threshold for prophylactic platelet transfusion to between 10 and 20 x109/L in patients judged to have additional risk factors for bleeding. Individual review is required.
What is the most common reason for platelet refractoriness?
Corrected count increment (CCI) At 24 hours post transfusion a CCI less than 5000 suggests platelet refractoriness.
How do I transfuse SDP?
Administration Of Platelets Procure platelets from the blood bank only prior to transfusion. Infuse platelet immediately upon arrival to the hospital. DO NOT STORE PLATELETS IN HOSPITAL REFRIGERATOR. Administer Platelets through a separate IV line.
What is RDP platelet?
It becomes necessary to collect blood from many donors and consolidate the Platelets obtained from each donor. Therefore, Platelets obtained from Whole Blood in routine blood donations are called Random Donor Platelets (RDPs). They are also called as “Pooled Platelets”.
What is Prbc in medical terms?
Packet red blood cell (PRBC), prepared by removing plasma from whole blood, is typically used to transfuse anemia patients who require infusion of red blood cell (RBC) to restore tissue oxygenation.
What is the other name of the platelets?
Platelets, also known as thrombocytes, are blood cells. They form in your bone marrow, a sponge-like tissue in your bones.
What is the other main indication for platelet transfusion?
1. Platelet transfusion is indicated for patients with clinically significant bleeding in whom thrombocytopenia is thought to be a major contributory factor, even if the platelet count is >10×109/L. 2. In patients with critical bleeding requiring massive blood transfusion.
What does platelet refractoriness mean?
Platelet refractoriness is defined as a repeated suboptimal response to platelet transfusions with lower-than-expected posttransfusion count increments. Refractoriness can be caused by immune and nonimmune factors, with nonimmune factors (Table 1) responsible for 60% to 80% of cases.
What is SDP transfusion?
The Platelets so collected are called Single Donor Platelets (SDP). Single Donor Platelets, being collected by a more efficient system of component separation, have a lesser chance of carrying other components like RBCs. They therefore become available to be transfused to a patient with any blood group.
Who can donate SDP?
Donors were selected based on following criteria: (i) Weight > 50 kg. (ii) Age – 18 to 60 years. (iii) At least three months from last donation/three days from last plateletpheresis.
What are the treatment options for Grade 1b aplastic anaemia?
Patients with iron overload after successful HSCT should undergo venesection. Grade 1B Aplastic anaemia patients who are severely neutropenic should be given prophylactic antibiotics and antifungal therapy according to local policies. Grade 2B
What is included in prophylaxis for aplastic anaemia in immunosuppressive therapy?
Aplastic anaemia patients receiving immunosuppressive therapy (IST) should also receive prophylactic anti‐viral agents, although routine prophylaxis against Pneumocystis jirovecii is not necessary. Grade 2C
When is a stem cell transplant recommended for patients with anemia?
Patients with severe or very severe aplastic anemia aged >35-50 years The British guidelines recommend up-front hematopoietic stem cell transplant (HSCT) for young and adult patients who have an MSD.
How is anaemia with hypocellular bone marrow diagnosed?
It is defined as pancytopenia with a hypocellular bone marrow in the absence of an abnormal infiltrate or marrow fibrosis. To diagnose AA there must be at least two of the following (Camitta et al, 1975) haemoglobin concentration (Hb) <100 g/l, platelet count <50 × 10 9 /l, neutrophil count <1·5 × 10 9 /l.