What is the primary deficiency in hyaline membrane of the newborn?
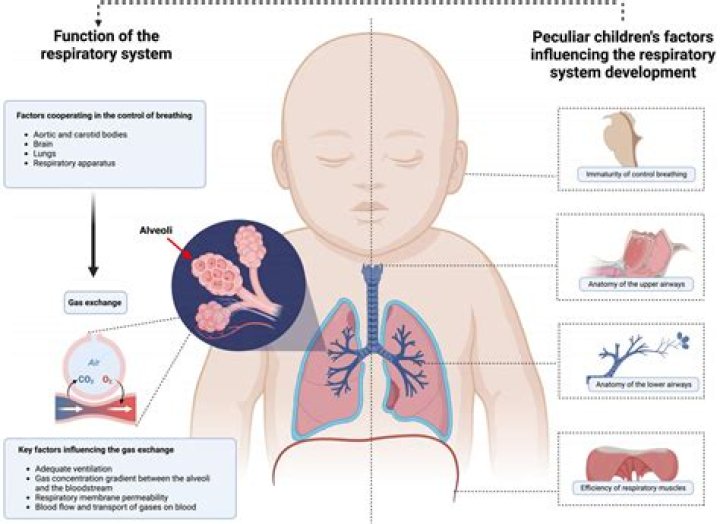
Hyaline membrane disease is now commonly called respiratory distress syndrome (RDS). It is caused by a deficiency of a molecule called surfactant. RDS almost always occurs in newborns born before 37 weeks of gestation. The more premature the baby is, the greater is the chance of developing RDS.
What causes RDS in newborns?
Neonatal RDS occurs in infants whose lungs have not yet fully developed. The disease is mainly caused by a lack of a slippery substance in the lungs called surfactant. This substance helps the lungs fill with air and keeps the air sacs from deflating. Surfactant is present when the lungs are fully developed.
Is hyaline membrane disease fatal?
Thus, it may be estimated that HMD was involved in the demise of nearly 12,000 neonates per year over this period. This amounts to approximately 20% of all neonatal deaths. On the basis of mortality rates, a trend toward an increased incidence of fatal HMD/RDS was established from 1968 to 1973.
How is respiratory distress syndrome diagnosed in newborns?
Diagnosing NRDS blood tests to measure the amount of oxygen in the baby’s blood and check for an infection. a pulse oximetry test to measure how much oxygen is in the baby’s blood using a sensor attached to their fingertip, ear or toe. a chest X-ray to look for the distinctive cloudy appearance of the lungs in NRDS.
How do you diagnose hyaline membrane disease?
HMD is usually diagnosed by a combination of assessments, including:
- appearance, color, and breathing efforts (these signs indicate your baby’s need for oxygen)
- x-rays of lungs: x-rays are electromagnetic energy used to produce images of bones and internal organs onto film.
How do premature babies get surfactant?
Methods to deliver surfactant The surfactant is administered via a thin catheter into the trachea in small aliquots, while the baby is spontaneously breathing on CPAP support. In infants 29-32 weeks gestation, LISA may reduce the occurrence of pneumothorax and need for mechanical ventilation.
What are the signs of RDS?
What are the symptoms of RDS?
- Respiratory difficulty at birth that gets progressively worse.
- Cyanosis (blue coloring)
- Flaring of the nostrils.
- Tachypnea (rapid breathing)
- Grunting sounds with breathing.
- Chest retractions (pulling in at the ribs and sternum during breathing)
How long does it take for surfactant to work?
Many babies start to get better within 3 to 4 days, as their lungs start to make surfactant on their own. They’ll start to breathe easier, look comfortable, need less oxygen, and can be weaned from the support of CPAP or a ventilator.
How is RDS diagnosed?
RDS is usually diagnosed by a combination of assessments, including the following: Appearance, color, and breathing efforts (indicate a baby’s need for oxygen). Chest X-rays of lungs. X-rays are electromagnetic energy used to produce images of bones and internal organs onto film.
What does hyaline membrane disease look like?
Hyaline Membrane Disease. Diffuse ground-glass appearance to both lungs with multiple air bronchograms (black arrows). An orogastric tube and umbilical venous catheter are present. Hyaline Membrane Disease. Diffuse ground-glass appearance to both lungs with hypoaeration and multiple air bronchograms.
What causes diffuse ground glass in the lungs?
Diffuse ground-glass appearance to both lungs with a left-sided tension pneumothorax and pneumomediastinum (orogastric tube is in distal esophagus) Hyaline Membrane Disease. Diffuse ground-glass appearance to both lungs with multiple air bronchograms (black arrows).
What are the signs and symptoms of a cyanotic infant?
The infant is cyanotic and requires CPAP immediately after delivery. He has subcostal retractions, grunting, and nasal flaring. Auscultation reveals decreased air entry in the lung fields throughout. Temperature is 98.2°F (36.8°C), pulse is 175 beats per minute, and respiratory rate is 70 breaths per minute. He requires an Fi o 2 of 0.4.
What tests are used to diagnose hyperchloremic membrane disease (HMD)?
In HMD, they often show a unique “ground glass” appearance called a reticulogranular pattern. blood gases (tests for oxygen, carbon dioxide, and acid in arterial blood): often show lowered amounts of oxygen and increased carbon dioxide. echocardiography (EKG): may be used to rule out heart problems that could cause symptoms similar to HMD.